The goal of the Chui SAMS Lab is to improve medication safety in the pharmacy setting by developing a more solid conceptual foundation for understanding medication errors in community pharmacies.
There are approximately 88,000 pharmacies across the United States dispensing 87.5 million prescriptions each week. Pharmacists support the health of patients and the public by:
Unfortunately, pharmacies can be chaotic work environments where any pharmacist would struggle to manage the day-to-day activities of taking care of patients and filling prescriptions. It is critically important to prevent medication errors that occur in the pharmacy.
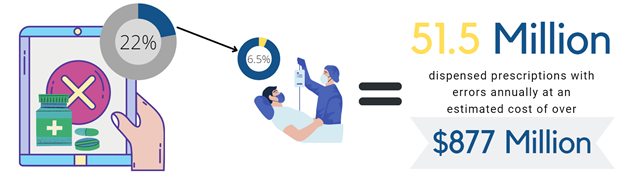
Medication dispensing errors negatively impact patients and pharmacists, resulting in either adverse drug experiences for the patient and/or increased pharmacy workload to correct the issue. Pharmacists do their best to manage such errors, but they have limited:
In order to reduce medication errors in community pharmacies, we must first develop a deep understanding of underlying reasons that lead to errors in the first place. By understanding these underlying reasons, we can most importantly use evidence to shift the (inappropriately placed) blame away from humans—as patients, providers, employees—to the system within which they operate.
The Chui SAMS Lab applies concepts from the scientific disciplines of human factors engineering (HFE) and industrial and health systems engineering, to improve patient safety in the community pharmacy setting. We are one of the first research groups to adopt HFE concepts beyond the hospital and primary care setting, to address medication safety in community pharmacies.
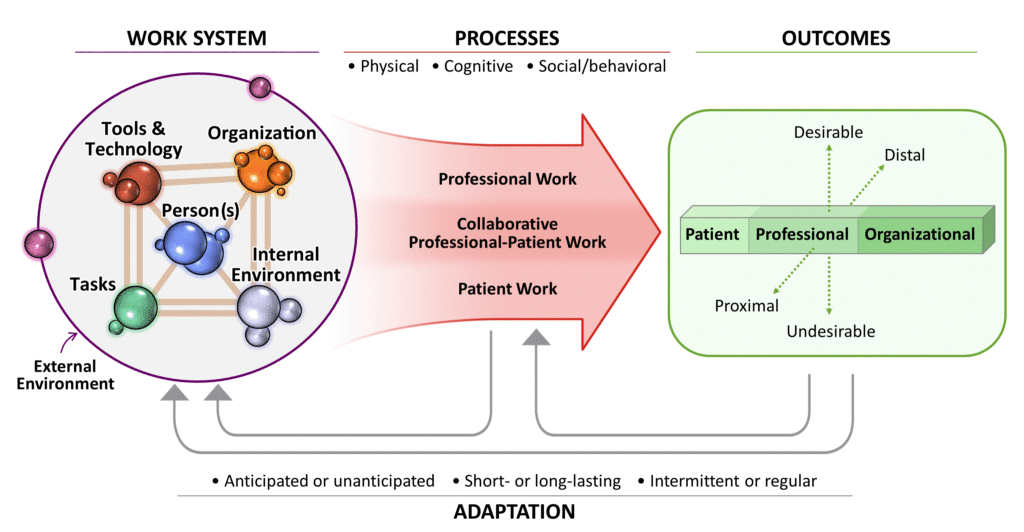
Human factors engineers have conceptualized a framework to examine key elements of a work system which include:
Work system elements interact to influence care processes, such as patient communication and counseling, which in turn impact both patient-specific outcomes, such as safety, and worker-specific outcomes, such as job satisfaction.
By applying HFE concepts to our research, we are able to look beyond the skills and knowledge of the individual pharmacist as the sole determinant of medication safety and focus on components of the work system as potential contributing factors to medication safety. We can explore work system influences that positively and/or negatively impact the work of pharmacists, which in turn, could influence medication safety.
Dr. Chui received UW–Madison School of Pharmacy Innovations in Technology Award
Dr. Chui Named Research in Social & Administrative Pharmacy Journal Top Reviewer
Dr. Chui accepted into ICTR KL2 Program
Dr. Chui Named Research in Social & Administrative Pharmacy Journal Top Reviewer
AHRQ grant awarded for “Improving Over the Counter Medication Safety for Older Adults”
Dr. Chui named Director of the Sonderegger Research Center
AHRQ grant awarded for “CancelRx: A Health IT Tool to Decrease Medication Discrepancies in the Outpatient Setting”
Dr. Chui named American Pharmacist Association (APhA) Fellow
Dr. Chui named Hammel-Sanders Distinguished Chair
AHRQ grant awarded for “Effectiveness and Sustainment of a Tailored Over-the-Counter Medication Safety Intervention in Community Pharmacies”
Dr. Chui named co-director of ICTR TL1 training program
Dr. Chui named Social & Administrative Sciences in Pharmacy Division Chair
AHRQ grant awarded for “Engineering Resilient Community Pharmacies (ENRICH)”
Dr. Chui named Vilas Distinguished Achievement Professorship
Awarded the 2024-2025 ICTR Pipeline Award for “Implementing an Intervention to Reduce Misuse of Over-the Counter Medications in Wisconsin for Hispanic/Latinx Older Adults: A Behind-the-Counter Approach”