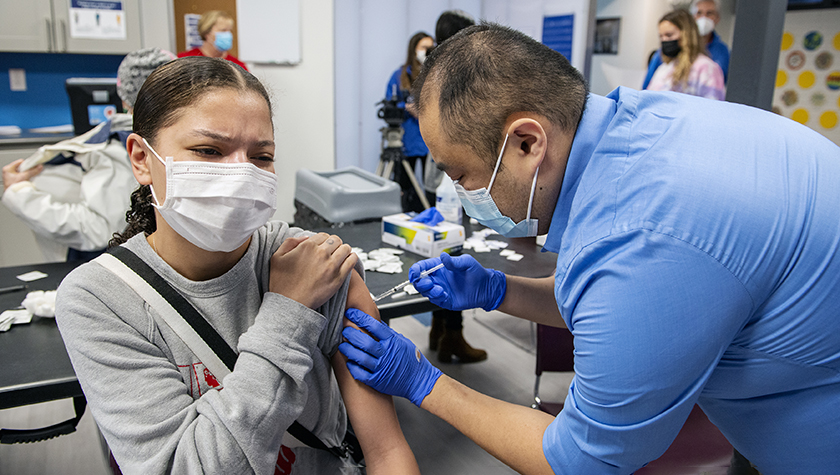
Multiple efforts at the School of Pharmacy aim to increase COVID-19 vaccine access and acceptance among BIPOC communities
By Katie Ginder-Vogel
“These dialogues are just the beginning,” says Mark Moua, a PharmD student at the University of Wisconsin–Madison School of Pharmacy.
Moua has been volunteering in several initiatives through the School to increase vaccination rates among BIPOC (Black, Indigenous, and people of color) communities, which often means having conversations to address questions and concerns about the vaccines.
“Their concerns and hesitations are valid,” he says. “These difficult conversations need to happen and be heard.”
“When we come into communities with a culturally humble lens, we show students the power of community outreach and why it’s important to build trust with patients.”
—Lisa Imhoff
In Wisconsin, about 44 percent of white residents have received at least one dose of a COVID-19 vaccine. For American Indian residents, that drops to just 29.5 percent — and even lower for Black populations, at 23.2 percent.
“Black and Indigenous people, and people of color, have suffered greater burdens of COVID-19 and are also potentially more skeptical of healthcare and therefore the vaccine,” says Mary Hayney, professor in the School of Pharmacy’s Pharmacy Practice Division.
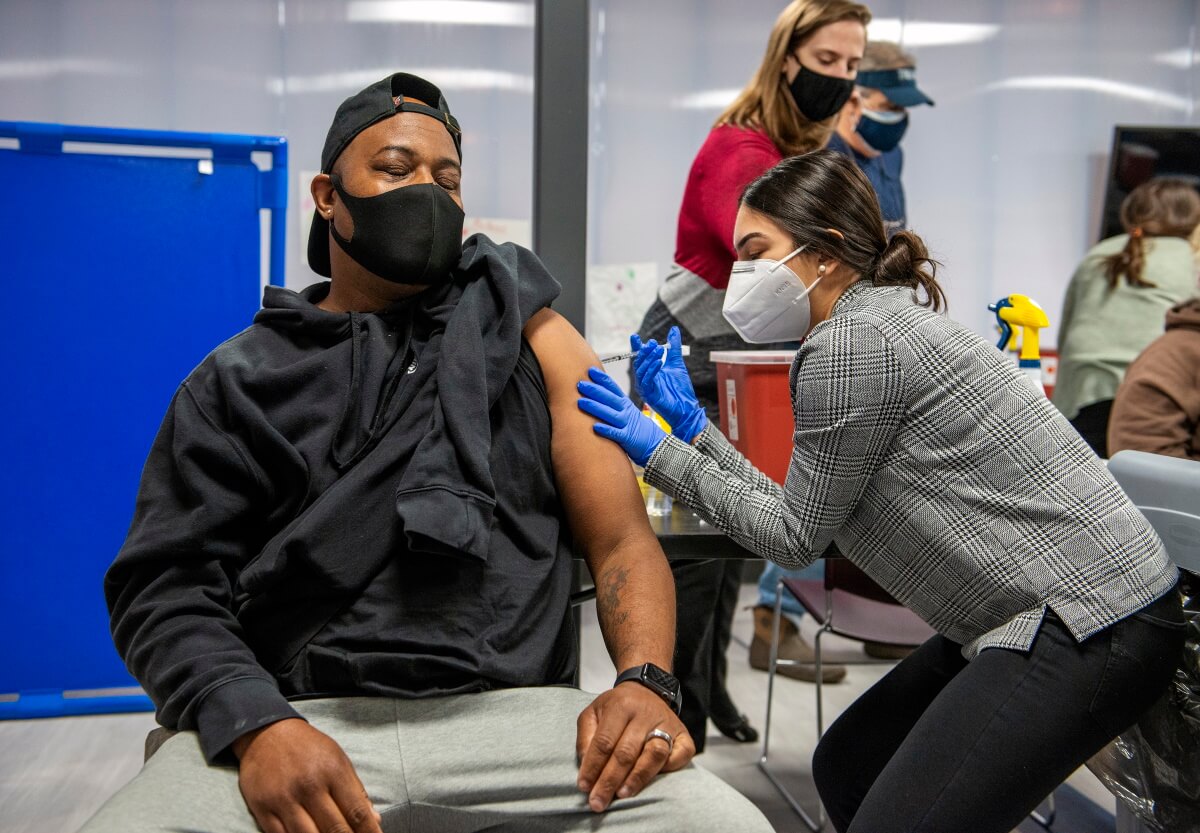
Members of the School of Pharmacy have been supporting three projects geared toward addressing those issues and reducing racial disparities in care. In one, the School of Pharmacy partnered with the Boys and Girls Club of Dane County to host a series of vaccine clinics and expert panel discussions. A second project, led by School of Pharmacy Professor Eva Vivian through her work with the African American Health Network of Dane County, is also using vaccine clinics and information campaigns in under-resourced Madison neighborhoods. The third opportunity sees students and faculty from the School volunteering in vaccine clinics organized by the Ho-Chunk Nation healthcare team.
Student pharmacists are playing a key role in all of these initiatives, and faculty at the School are equipping them to respectfully serve diverse populations through changes in the curriculum, including a new lecture about the history of racism in medical research. That context is key to relating to patients and earning trust, says Lisa Imhoff, associate dean for Diversity and Inclusion Initiatives at the School of Pharmacy.
“When we come into communities with a culturally humble lens, we show pharmacy students the power of community outreach and why it’s important to build trust with patients,” says Imhoff.
Reaching underserved communities
A new partnership between the UW–Madison School of Pharmacy, Fitchburg Family Pharmacy, and the Boys and Girls Club of Dane County makes steps toward rebuilding trust with communities of color and increasing access to the COVID-19 vaccine through a series of community-focused events, giving student pharmacists the chance to get involved as vaccinators.
Together, the School and the Boys and Girls Club hosted eight vaccine clinics in neighborhoods around Madison on Saturdays in April and May, providing vaccines to more than 600 community members. Although the vaccination clinics were designed to reach BIPOC community members, they were open to all Madison residents. Fitchburg Family Pharmacy provided the vaccine doses, and School of Pharmacy PharmD students helped administer them.

“I want to be a person of color here to help with people who may need translations,” says Tracy Lor, a third-year PharmD student who volunteered at the clinics. “The most satisfying part is being able to make people feel assured, answer any questions they have, and be here for whatever they need.”
In addition to the vaccine clinics, members of the School and the Boys and Girls Club also hosted two virtual town hall discussions on May 12 and 13 aimed at reducing vaccine hesitancy, featuring BIPOC healthcare professionals and community leaders, including Imhoff and School of Pharmacy Associate Professor Olayinka Shiyanbola. Panelists discussed the historical and contemporary reasons behind vaccine hesitancy in BIPOC communities, unequal healthcare access, the history of vaccines and how vaccines work, and their personal vaccination experiences.
“As someone who studies misinformation/beliefs and health literacy and as someone who identifies as Black and an immigrant, it was important to me to be there to talk about why I got vaccinated, and hopefully that relates to people in the community who are Black or immigrants and might be needing that information to help make their own informed decisions,” says Shiyanbola.
Cierra Brewer (PharmD ‘21) joined Shiyanbola and Imhoff at the youth-focused May 13 town hall that fielded questions from local teenagers.

“If you have mistrust or are nervous, based on what we’ve seen in the past, especially for people of color, that opinion is very valid,” Brewer says. “The more data we have, the more we can make the community feel comfortable. I want to provide them with the information they need to make an informed decision.”
This vaccine equity initiative reached the White House, with the Boys and Girls Club of Dane County CEO Michael Johnson, Fitchburg Family Pharmacy owner Thad Schumacher, and School of Pharmacy’s Imhoff landing an invitation to be panelists in a “State of Vaccines” webinar on June 16 that features the U.S. Surgeon General and hosted by the U.S. Department of Health and Human Services.
Addressing social determinants of health
Through her role as chair of the African American Health Network of Dane County (AAHN), School of Pharmacy Professor Eva Vivian is leading a broad community partnership to promote equity in COVID-19 vaccination among African American community members, which received grant funding from the Wisconsin Department of Health Services (DHS).
Vivian’s research and clinical practice have long focused on addressing health disparities and preventing disease by recognizing the breadth of factors that influence healthcare and health decisions, and those factors have been exacerbated by the pandemic.
“COVID-19 has exposed the disparities in our country and how structural racism has caused an uneven distribution of social determinants of health.”
—Eva Vivian
“As a pharmacist, I learned that so many things impact health outside the healthcare system — where people live, access to education, transportation, work environment, and so on — and healthcare providers have to be aware of these things to help people,” says Vivian, who was honored with the 2021 Healthy Aging Star Award for Health Equity from the Wisconsin Institute for Healthy Aging. “COVID-19 has exposed the disparities in our country and how structural racism has caused an uneven distribution of social determinants of health.”
In partnership with Dane County Public Health, the Goodman Community Center, the Lussier Community Center, and the Urban League, AAHN is offering 20 to 30 mobile education and vaccination programs across Madison from May through August — and that timeline may be extended into the fall.

The Goodman Community Center began hosting vaccine clinics, funded by the grant, in April, but Vivian and Goodman Center CEO Letesha Nelson felt they needed to do more community outreach and education to draw their target population: communities of color who are vaccine hesitant.
“We need people to understand the virus, the vaccine, and how it is going to make an impact in their communities,” says Nelson, who lost a family member to COVID-19. “We have to mobilize people in Madison — in every community.”
To help educate community members who might feel unsure about the vaccine, a Goodman Center representative and an AAHN volunteer went door-to-door in nearby neighborhoods, to connect with people and provide information about the vaccine, and Vivian offered an educational session at the Goodman Community Center.
“I understand why people are reluctant to get this vaccine, when you take into consideration everything that has gone on in our society and how people of color have been treated in their lifetimes,” says Vivian, who has been AAHN chair since 2013.
After the weeklong education and outreach effort, 26 people were vaccinated at the Goodman Community Center clinic on May 21, including a 15-year-old who worked with a Goodman staffer to review comprehensive information about the vaccine.
“I saw the look on her face when she got that vaccine card and the sense of pride that she was vaccinated,” adds Vivian. “You have to arm people with the education and knowledge to make an informed decision.”
Another clinic, a pop-up event in partnership with SSM Health and the Urban League of Greater Madison, vaccinated more than 60 community members, and more events are in the works.
“I think we’re going to have to be patient,” says Vivian. “Right now, we’re working with people who have had negative experiences with the healthcare system their entire lives, and I think they’re going to have to be convinced that it’s safe. When people who got vaccinated go home and tell their family, that may help.”

Vivian anticipates an extension from DHS and says that the partnership with Dane County Public Health will also allow AAHN to extend its outreach efforts beyond August to continue to reach community members. Nelson envisions a steady stream of small groups deciding to get vaccinated throughout the summer.
“We want to be ready to be able to respond when smaller groups come together and keep sharing information about our clinics,” says Nelson. “It takes education and time for people in our community to feel ready.”
Moua is one of the PharmD students who helped prepare vaccines at the first Goodman Center clinic and participated in efforts to answer neighbors’ questions about the vaccines. He says his greatest moment of growth from these clinics has been speaking with the community.
“We strive to establish trust within the community because we know it takes time to change perspectives,” he says. “We’re hoping to generate the discussion, and maybe they’ll reconsider after much thought. Sometimes, we don’t have answers for their questions but it’s more important to just listen.”
PharmD student Ugboaku Maryann Egbujor says volunteering at the Goodman Center clinics has helped her understand the importance of diversity and inclusion in healthcare.

“At the clinics, I got to appreciate the sense of ‘togetherness’ among diverse groups of people,” she says. “There is still more work to be done in creating inclusive groups of healthcare professionals, which may create a more trusting environment for individuals from various backgrounds and help encourage more people to get vaccinated.”
Vivian is proud to see the pharmacy students’ involvement and awareness of the health disparities in Dane County and nationally, as well as their ability to be agile and adjust to the community’s needs.
“It’s important for them to see that when things don’t go according to plan, we change the plan to better accommodate the people we most need to reach,” says Vivian.
Vaccinating tribal members
In the U.S., indigenous populations had higher rates of COVID-19 infection, hospitalization, and death than almost any other demographic group, with African American and Latinx populations similarly adversely affected, according to the Centers for Disease Control.

“The risk of COVID-19 infection, hospitalization, and death among Native/Indigenous, Hispanic, and Black populations, with white as a comparator, is striking,” says Hayney. She and PharmD students from the School have volunteered at several COVID-19 vaccine clinics organized by the Ho-Chunk Nation.
Jennifer Baird, an infection prevention and employee health nurse with the Ho-Chunk Nation, was formerly the manager of specialty clinics at UW–Madison’s University Health Services before joining the House of Wellness in 2017, and she worked with Hayney on the successful meningitis B immunization effort on campus in 2016, following the diagnosis of several students. In the face of another public health crisis, COVID-19, Baird contacted Hayney to recruit student pharmacist volunteers for clinics at the Ho-Chunk House of Wellness in Baraboo and the Ho-Chunk Nation District 1 Community Center in Black River Falls.
“They were awesome,” says Baird of the pharmacy student volunteers. “They’re always so helpful and so positive, and our patients even commented that they’re so glad to be part of their learning experience.”
“These were the first up-close and personal conversations with people I’ve had in a while, and it reminded me what I love about pharmacy: being an accessible resource for patients to help improve their health.”
—Jayne Hurd
“The Ho-Chunk Nation healthcare staff has done a fantastic job getting people through its vaccine clinics really quickly,” says Hayney. “For example, on April 28, they had 1,200 appointments.”
So far, the Ho-Chunk Nation has delivered more than 16,000 doses to tribal members, employees, and community members. And about 60 percent of tribal elders are fully vaccinated.
“That’s good, but not good enough, because the other 40 percent are high risk,” she says. “The lowest category of vaccinated individuals is young — 22 to 35 — so we’re figuring out how to get those numbers up.”

Jayne Hurd (PharmD ‘21) — who as a pharmacy student volunteered for vaccination clinics at Fitchburg Family Pharmacy, one for teachers in Mt. Horeb, at Boscobel Pharmacy, and in her hometown of Portage — used a personal day to volunteer at the Ho-Chunk House of Wellness.
“These were the first up-close and personal conversations with people I’ve had in a while, and it reminded me what I love about pharmacy: being an accessible resource for patients to help improve their health,” she says. “For communities with less access to preventative care, it was a great opportunity to educate people about the COVID vaccine and the flu vaccine.”
Hurd even helped one hesitant patient change his mind and agree to be vaccinated against COVID-19. “I felt really good because he had questions, and I felt like I had the answers,” she says. “He was ready to listen, took the shot, and thanked me for the information.”

Fourth-year PharmD student Natasha Virrueta, who has also been volunteering weekly at Fitchburg Family Pharmacy, appreciated the chance to work with a different patient population outside Madison.
“From a public health perspective, it was really cool to see a large, well-run clinic in a rural community,” says Virrueta. “It’s made me think about how I interact with each individual patient and make sure I’m doing a great job for people who may not have as much access to care,” she says.
Samantha Lewiston (PharmD ‘21), who has also volunteered at numerous vaccine clinics, spent a full day volunteering at the House of Wellness and estimates she administered 100 vaccines.
“It was energizing, talking to patients, who were all so grateful,” says Lewiston. “I had a couple of pregnant patients who were very excited because they had talked with their doctors and discussed the benefits and risks and were finally able to come get a vaccine to protect themselves and likely pass protection to the baby. I was giving one vaccine and protecting two people.”
“There is much more that we at the School of Pharmacy can do to address hesitancy, and I think that’s going to be done personally — with personal conversations to truly address the questions — all summer long, into fall.”
—Mary Hayney
Lewiston noted that COVID has brought many of the inequities of healthcare access for rural and indigenous populations to light.

“Volunteering becomes an even larger piece of the puzzle when talking about getting healthcare to those populations because of the lack of resources to support hired healthcare personnel to get shots into arms,” says Lewiston.
The impact of these initiatives will be felt around the state of Wisconsin, but Hayney reiterates that there is more work to be done, in each patient interaction and in the classroom.
“There is much more that we at the School of Pharmacy can do to address hesitancy, and I think that’s going to be done personally — with personal conversations to truly address the questions — all summer long, into fall,” says Hayney.




